Caring for a loved one with limited mobility in the heart of New York City presents a unique set of challenges that can feel overwhelming for any family. We understand that your priority is keeping your parent or relative comfortable and safe within the familiar surroundings of their own home. Our specialized nursing approach focuses on providing the highest standard of clinical care while empowering your family with the knowledge needed to maintain skin integrity. By bringing professional expertise directly to your doorstep, we bridge the gap between hospital-grade treatment and the comfort of home life.
Clinical Quick Answer
Effective wound care in a residential setting requires a proactive strategy led by a wound management nurse NYC home specialist who focuses on both active treatment and rigorous Bed Sore Prevention. Utilizing advanced pressure-redistribution surfaces, moisture-barrier protocols, and medical-grade dressings ensures that skin remains intact even for bedbound patients. Professional RN oversight is critical for identifying early-stage pressure injuries before they escalate into complex, life-threatening infections.
The Critical Role of a Wound Management Nurse NYC Home Specialist
- Comprehensive Skin Assessments: A specialized nurse performs head-to-toe evaluations to detect microscopic changes in skin health that an untrained eye might miss, particularly in areas prone to friction.
- Personalized Care Mapping: Every NYC apartment is different; your nurse creates a customized plan that accounts for your specific furniture layout, caregiver availability, and the patient’s unique medical history.
- Advanced Debridement and Dressing: For existing wounds, the nurse applies clinical expertise to remove necrotic tissue and select moisture-retentive dressings that facilitate autolytic healing.
- Medication Management: Monitoring for signs of systemic infection and coordinating with primary care physicians to adjust antibiotics or pain management protocols as healing progresses.
- Caregiver Coaching: Training family members on proper transfer techniques and the use of sliding sheets to minimize the shearing forces that lead to skin tears.
- Coordination of Supplies: Managing the logistics of ordering medical-grade supplies through NYC insurance providers to ensure you never run out of essential barriers or bandages.
Bed Sore Prevention: Strategies for NYC Residents
- The Rule of 2-Hour Repositioning: Implementing a strict turning schedule-shifting the body’s weight every two hours-to prevent prolonged pressure on the sacrum, hips, and heels.
- Microclimate Management: Keeping the skin at an optimal temperature and moisture level; excessive sweat or incontinence-related moisture is a primary driver of skin breakdown.
- Heel Elevation Protocols: Using “floating” techniques where pillows or foam wedges are placed under the calves to ensure the heels have zero contact with the bed surface.
- Nutritional Fortification: Ensuring the patient receives adequate protein, Vitamin C, and Zinc, which are the building blocks of skin repair and resilience.
- Hydration Monitoring: Dehydrated skin is thinner and more prone to cracking; nurses monitor fluid intake to maintain skin turgor and elasticity.
Navigating NYC Apartment Challenges for Skin Care
- Space Optimization: NYC apartments often have narrow hallways and small bedrooms; a wound management nurse NYC home expert helps rearrange the environment to allow for hospital bed placement and easy 360-degree patient access.
- Radiator Safety: Many older NYC buildings rely on steam heat; nurses identify and mitigate the risk of “radiator burns” for patients with neuropathy who may not feel the heat against their skin.
- Humidity Control: NYC summers can be stifling and winters dry; nurses advise on using humidifiers or air conditioners to prevent the skin from becoming too brittle or too macerated.
- Flooring and Mobility: Assessing area rugs and floor transitions to prevent falls during transfers, which are a major cause of skin trauma in the elderly.
- Lighting for Inspection: Ensuring the care area has high-quality lighting so that caregivers can accurately check for the subtle “pinkness” of a Stage 1 pressure injury.
- Elevator and Access Logistics: Coordinating with building management for the delivery of heavy medical equipment like hoyer lifts or specialized bariatric beds.
The Clinical Stages of Pressure Injuries
- Stage 1: Non-Blanchable Erythema: The skin is intact but stays red or purple when pressed. This is the “warning” stage where Bed Sore Prevention efforts must be intensified.
- Stage 2: Partial-Thickness Skin Loss: The top layer of skin (epidermis) is lost, often looking like a shallow open ulcer or a fluid-filled blister.
- Stage 3: Full-Thickness Skin Loss: The wound extends into the fatty tissue layer (subcutaneous), creating a crater-like appearance that requires professional packing and cleaning.
- Stage 4: Full-Thickness Tissue Loss: Deep damage extending to the muscle, tendon, or bone; these wounds carry a high risk of osteomyelitis and require intensive nursing intervention.
- Unstageable Wounds: Covered by slough (yellow/tan) or eschar (black/brown), making it impossible to see the depth; these must be debrided by a professional.
- Deep Tissue Pressure Injury: Persistent non-blanchable deep red or maroon discoloration that may evolve rapidly into a full-thickness wound.
Interdisciplinary Coordination with NY State Resources
- NYC DOH Guidelines: Adhering to the latest safety and hygiene standards set by the NY State DOH to ensure all home-based care meets state-level quality benchmarks.
- MLTC Communication: Working closely with Managed Long-Term Care (MLTC) plans to justify the necessity of increased nursing hours for high-risk wound patients.
- Home Health Aide (HHA) Supervision: The RN trains the HHA on specific skin-prep routines and how to document changes in wound exudate or odor daily.
- Telehealth Integration: Utilizing secure photo sharing and video calls to provide real-time consultations with wound care doctors and surgeons between home visits.
- Equipment Procurement: Navigating the complex NYC medical supply chain to get high-tech dressings and vacuum-assisted closure (VAC) therapy units delivered directly to the apartment.
- Social Work Support: Connecting families with local NYC support groups to manage the emotional toll of long-term caregiving for a bedbound relative.
Advanced Treatment Modalities Used in Home Settings
- Negative Pressure Wound Therapy (NPWT): Using a vacuum-sealed dressing to pull excess fluid out of the wound and stimulate the growth of new granulation tissue.
- Silver and Honey Dressings: Utilizing antimicrobial properties of medical-grade silver or Leptospermum honey to combat antibiotic-resistant bacteria locally.
- Collagen Matrix Fillers: Applying bovine or avian collagen to the wound bed to provide a scaffold for the patient’s own skin cells to grow across.
- Enzymatic Debridement: Using chemical ointments that selectively dissolve dead tissue while leaving healthy tissue untouched, avoiding the need for surgical intervention.
- Hydrocolloid and Foam Barriers: Strategic use of dressings that provide a “second skin” to protect high-friction areas like the sacrum from friction and shear.
- Compression Therapy: For wounds on the lower legs caused by venous insufficiency, nurses apply specialized multi-layer wraps to improve circulation and reduce swelling.
Nurse Insight: In my experience working with families in Manhattan and Brooklyn, the biggest hurdle to Bed Sore Prevention isn’t a lack of love, but a lack of space. In tight NYC apartments, we often find that the bed is pushed against a wall, making it nearly impossible to turn the patient to one side. My first piece of advice is always to move the bed to the center of the room, even if it feels awkward at first. This 360-degree access allows for proper repositioning and thorough skin checks that literally save lives by preventing deep-tissue infections.
Frequently Asked Questions
How can I tell if a red spot is a bed sore or just a temporary mark?
Use the “blanch test”: press your finger firmly on the red spot for a few seconds. If the skin turns white (blanches) and then turns back to red when you let go, circulation is still good. If the spot stays red and does not turn white, it is likely a Stage 1 pressure injury, and you should contact your wound management nurse NYC home specialist immediately.
Why are heels so vulnerable to skin breakdown in bedbound patients?
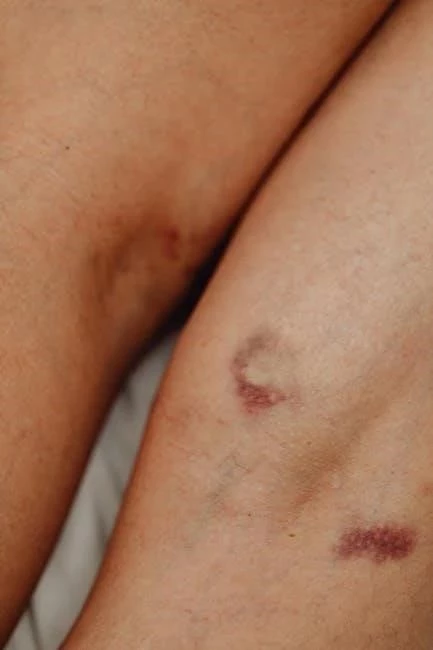
The skin over the heel is very thin, and there is very little fat or muscle to cushion the bone. When a patient lies on their back, the entire weight of the leg often rests on that tiny point of the heel, cutting off blood flow quickly. This is why “floating the heels” with pillows is a cornerstone of Bed Sore Prevention.
Is a hospital bed necessary for home-based wound care?
While not always mandatory, a hospital bed is highly recommended because it allows you to adjust the head and foot of the bed. This helps prevent the patient from sliding down, which causes “shearing”-a process where the skin stays in place while the bone moves, tearing the underlying blood vessels.
Can poor nutrition cause wounds to stop healing?
Yes. The body requires a massive amount of energy and protein to knit skin back together. If a patient is malnourished, the body will prioritize vital organs over skin repair. A nurse will often recommend high-protein supplements and specific vitamins to “fuel” the healing process from the inside out.
How do I manage a wound if the patient is also incontinent?
Incontinence is a major risk factor because moisture weakens the skin. We use specialized moisture-barrier creams (zinc-based or dimethicone) and high-absorbency briefs that wick moisture away from the skin. A wound management nurse will teach you a “cleanse, protect, and monitor” routine for every change.
Contact ProLife Home Care NYC for a free clinical assessment:(718) 232 – 2777
Contact ProLife Home Care NYC for a free clinical assessment: (718) 232-2777